The Facts on Heel Pain:
Heel Pain 101
Heel pain is pain in the heel area that can vary in severity and location. It is most common in adults.
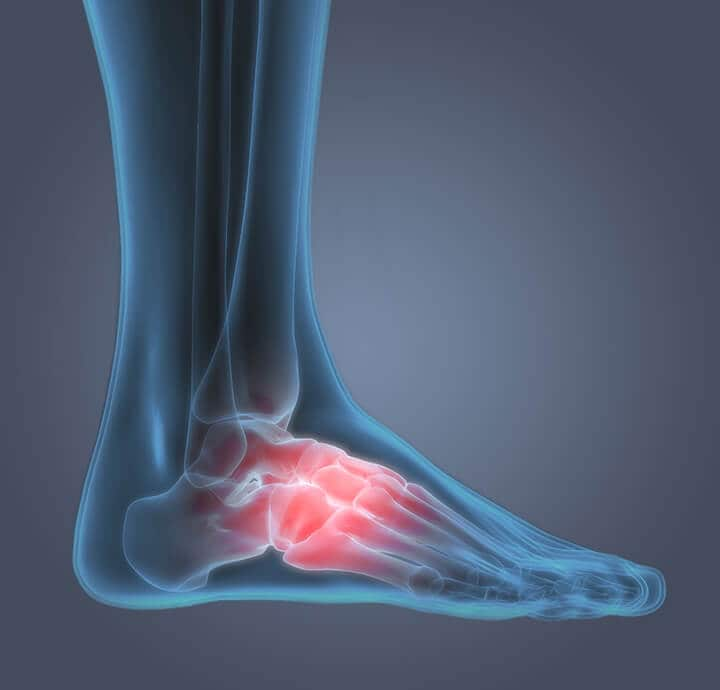
The heel is the first bone to contact the ground when walking and takes the full force of impact and the resulting shock of bearing weight during motion, resulting sometimes in sore heel pain. General heel pain tends to dissipate overnight and can reappear or worsen during prolonged periods of walking or standing.
The pain is commonly intense when getting out of bed or a chair but often lessens when walking – although that is more common in the case of Plantar Fasciitis.
What Causes Heel Pain?
One common cause of heel pain is plantar fasciitis. Plantar fasciitis involves stretching of the plantar fascia, a ligament that runs from the ball of foot through the arch and is attached to the heel which becomes aggravated and causes pain in your heel. One way to tell if your heel pain is plantar fasciitis is whether the pain is more acute first thing in the morning and then fades.
Heel spurs, which are abnormal bone growths coming off the heel, can also cause heel pain. Other causes include repetitive stress or shock to the heel, standing for prolonged periods and osteoarthritis.
Shop Products for Heel Pain
DON'T LET ARCH PAIN SLOW YOU DOWN
IF YOU HAVE HEEL PAIN, RELIEF IS POSSIBLE. JUST A FEW STEPS THAT CAN HELP INCLUDE:
- Place insoles or inserts in your shoes to help control abnormal foot motion
- Wear properly fitting shoes
- Maintain a healthy weight
- Make sure you give your body time to warm up when you exercise, and practice good stretching techniques
Not a medical diagnosis. For information purposes only. If you have diabetes, poor blood circulation, or fragile skin, or symptoms are severe or persist, consult your podiatrist or physician before using products.